Catalog № 051-322
For in vitro diagnostic use
For professional use only
Please read the instructions carefully before use
INTENDED USE The Coronavirus Diseases 2019 (COVID-19) IgM/IgG Antibody Test is a rapid, qualitative and convenient immunochromatographic in vitro assay for the differential detection of IgM & IgG antibodies to COVID-19 virus in human serum, plasma or whole blood samples obtained from patient with COVID-19 infection. The device is designed to aid in the determination of recent or previous exposure to COVID-19 virus tracking the status of the disease after COVID-19 Virus infection.This assay only provides a preliminary result. A positive result does not necessarily mean a current infection, but represents a different stage of the disease after infection. IgM positive or IgM/IgG both positive suggest recent exposure, while IgG positive suggests previous infection, or latent infection. Current infection should be confirmed by Real-Time Reverse Transcriptase (RT-PCR) or viral gene sequencing. The test is intended for professional use.
SUMMARY
Since late December, 2019, an outbreak of a novel coronavirus disease (COVID-19; previously known as 2019-nCoV) was reported in Wuhan, China, which has subsequently affected 190 countries worldwide. In general, COVID-19 is an acute resolved disease but it can also be deadly, with a 2% case fatality rate. Severe disease onset might result in death due to massive alveolar damage and progressive respiratory failure. The pathogen has since been identified as a zoonotic coronavirus, similar to SARS coronavirus and MERS coronavirus, and has been named as severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2).
The 2019 novel coronavirus (SARS-CoV-2) epidemic has been declared a public health emergency of international concern by the World Health Organization, may progress to a pandemic associated with substantial morbidity and mortality. SARS-CoV-2 is genetically related to SARS-CoV, which caused a global epidemic with 8096 confirmed cases in more than 25 countries in 2003.
TEST PRINCIPLE
The principle of COVID-19 IgM/IgG Antibody Test is an antibody-capture immunochromatographic assay for the simultaneous detection and differentiation of IgM & IgG antibodies to COVID-19 virus in human serum, plasma, or whole blood samples. COVID-19 virus-specific antigens are conjugated to a colloidal gold and deposited on the conjugate pad. Monoclonal anti-human IgM and monoclonal anti-human IgG are immobilized on two individual test lines (T2 and T1) of the nitrocellulose membrane. The IgM line (T2) is closer to the sample well and followed by the IgG line (T1). When the sample is added, the gold-antigen conjugate is rehydrated and the COVID-19 IgM and/or IgG antibodies, if any in the sample, will interact with the gold conjugated antigen. The immunocomplex will migrate towards the test window until the test zone (T1 & T2) where they will be captured by the relevant anti-human IgM (T2) and/or anti-human IgG (T1), forming a visible pink line, indicating positive results. If COVID-19 antibodies are absent in the sample, no pink line will appear in the test lines (T1 & T2), indicating a negative result.
To serve as an internal process control, a control line should always appear at Control Zone (C) after the test is completed. Absence of a pink control line in the Control Zone is an indication of an invalid result.
REAGENTS AND MATERIALS PROVIDED
- Pouch contents: Test Cassette, Desiccant.
- 25 Capillary tubes (20 µl) for 25 tests.
- Sample buffer (3 ml) per bottle for 25 tests.
- Test instruction.
MATERIALS REQUIRED BUT NOT PROVIDED
- Alcohol swab.
- Lancet and blood collection device.
- 0.5µl-20µl pipette
- Gloves.
- Clock or timer.
STORAGE AND STABILITY
The COVID-19 IgM/IgG Test device is to be stored refrigerated or at room temperature (2-30°C) under dry conditions for the duration of its shelf life. The test device is stable through the expiration date printed on the sealed pouch. The test device must remain sealed in the pouch until use.
DO NOT FREEZE.WARNINGS AND PRECAUTIONS
- For professional in vitro diagnostic use only. Do not reuse.
- Do not use if the product seal or its packaging is compromised.
- Do not use after the expiration date shown on the pouch.
- Do not mix and interchange different specimens.
- This test should be performed at 15 to 30°C (59 to 86°F). If stored refrigerated, ensure that the Test Units are brought to operating temperature before performing testing.
- Wear protective clothing such as laboratory coats, disposable gloves and eye protection while handling potentially infectious materials or performing the assay.
- Wash hands thoroughly after finishing the tests.
- Do not eat, drink or smoke in the area where the specimens or kits are handled.
- Clean up spills thoroughly with appropriate disinfectants.
- Handle all specimens as if they contain infectious agents. Observe established precautions against microbiological hazards throughout testing procedures.
- Dispose of all specimens and used devices in a proper bio-hazard container. The handling and disposal of the hazardous materials should follow local, regional or national regulations.
- Keep out of children’s reach.
SPECIMEN COLLECTION AND STORAGE
For Whole Blood Samples:The whole blood samples may be collected by fingerstick or venipuncture, following routine facility procedures. In summary:
Fingerstick whole blood:- Clean the area of finger to be lanced with the alcohol swab. Allow to dry.
- Without touching the puncture site, rub down the hand towards the middle or ring finger fingertip.
- Puncture the skin with a sterile lancet and wipe away the first drop of blood.
- Gently rub the hand from wrist to the lanced finger to form a full drop of blood over the puncture site.
- Collect the blood droplet using the included capillary tube.
- Fingerstick whole blood must be tested immediately after collection.
- Collect venous whole blood in a tube with anticoagulant.
- Whole blood samples should be tested immediately after sample collection.
For Serum samples, collect blood in a tube without anticoagulant and allow it to clot.
For Plasma samples, collect blood in a tube containing anticoagulant.
- Separate serum or plasma from blood as soon as possible to avoid hemolysis. Use only clear, non-hemolyzed specimens.
- The blood may be stored at 2ºC to 8ºC for up to three days if the tests cannot be performed immediately. Allow sample to attain room temperature (without heating) prior to use.
ASSAY PROCEDURE
- Remove the testing device from the sealed pouch by tearing at the notch and place the testing device on a flat, dry surface.
- For fingerstick or venous whole blood:
Using a capillary tube, collect the fingerstick whole blood or whole blood (20µl) till the black line.
For serum/plasma:
Using a pipette, collect the serum/plasma (10µl). - Add the collected serum/plasma/whole blood to upper area (close to test window) of sample well on the test device without air bubbles (hold the capillary tube/ pipette vertically and gently touch the end against the pad within the sample well for transferring).
- Wait for 20-30 seconds; add 2 drops (around 90µl) of the sample buffer to the Sample Well of the test device.
- Read the results after 15-30 minutes. Strong positive specimens may produce positive result in as little as 1 minute.
Note: In order to prevent an incorrect reading, do not read the test results after 30 minutes. If the test is read after 30 minutes, the intensity of the colored lines may change or a new line may appear. To avoid confusion, discard all test devices after interpreting results.
INTERPRETATION OF RESULT
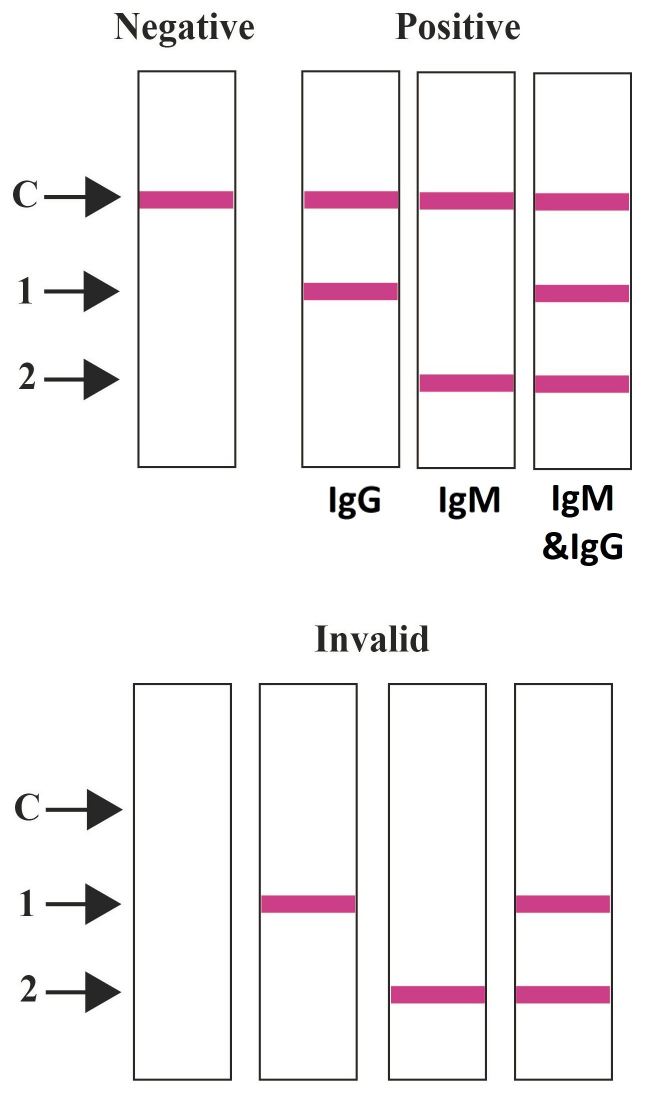
Positive:Pink colored bands appear at the control region (C) and T1 and /or T2 region.IgM and IgG Positive, visible bands at T2 and T1, indicating positive result for a possible COVID-19 infection.
IgM positive, a visible band at T2 region, indicating positive result for a possible COVID-19 infection.
IgG positive, a visible band at T1 region, indicating a positive result for a possible COVID-19 infection.
Negative:A pink colored band appears only at the control region (C), indicating a negative result for COVID-19 infection. Invalid:
No visible band at the control region (C). Repeat with a new test device. If test still fails, please contact the distributor with the lot number.
AFTER TESTING
The specimens may be potentially infectious. Avoid contact with skin by wearing gloves and proper laboratory attire. Properly handle and dispose of all test devices in an approved biohazard container. Residual sample should be disposed of in a medically approved manner after completion of all testing.
QUALITY CONTROL
The COVID-19 IgM/IgG Test devices have a built-in process Control Region (C). A pink band should always appear in this region regardless of the presence of IgM & IgG antibodies to COVID-19 virus in sample. This pink process Control band verifies: 1) that sufficient serum volume was added, 2) that proper flow is obtained, and 3) that the reagents worked properly. If this band is missing, the test was not performed correctly or failed to function correctly. Such a test is inconclusive and the specimen should be repeated using a new test device.
Good laboratory practice recommends the daily use of an outside control to ensure proper testing device performance. Quality control samples should be tested according to the standard quality control requirements established by your laboratory. When testing the quality control standards, use the same assay procedure as with a serum or whole blood sample. It is recommended that control specimens be used for each new lot of kits.
PERFORMANCE CHARCATERISTICS
The sensitivity and specificity of COVID-19 IgM/IgG Antibody Test: Total 460 samples were evaluated for sensitivity and specificity. Chemiluminescent immunoassay (CLIA) was used as reference method. It showed that COVID-19 IgM/IgG Antibody Test had good correlation with CLIA.
| COVID-19 IgM/IgG Antibody Test (IgM) | ||||
| Positive | Negative | Total Result | ||
| CLIA | Positive | 72 | 4 | 76 |
| Negative | 5 | 379 | 384 | |
| Total Result | 77 | 369 | 460 | |
| Sensitivity and Specificity | Sensitivity: 72/76 (97.37%) Specificity: 379/384 (98.70%) | |||
| COVID-19 IgM/IgG Antibody Test (IgG) | |||||
| Positive | Negative | Total Result | |||
| CLIA | Positive | 84 | 6 | 90 | |
| Negative | 6 | 364 | 370 | ||
| Total Result | 76 | 370 | 460 | ||
| Sensitivity and Specificity | Sensitivity: 71/76 (93.33%) Specificity: 364/370 (98.38%) | ||||
LIMITATIONS
- Humidity and temperature can adversely affect results.
- The instructions for the use of the test should be followed during testing procedures.
- There is always a possibility that false results will occur due to the presence of interfering substances in the specimen or factors beyond the control of the manufacturer, such as technical or procedural errors associated with the testing.
- Although the test demonstrates superior accuracy in detecting antibodies against COVID-19 virus, a low incidence of false results can occur. Therefore, other clinically available tests are required in case of questionable results. As with all diagnostic tests, a definitive clinical diagnosis should not be based on the results of a single test, but should only be made by the physician after all clinical and laboratory findings have been evaluated.
- Clinical management of severe acute respiratory infection (SARI) when COVID-19 disease is suspected, Interim guidance, World Health Organization, 13 March 2020.
- Report of the WHO-China Joint Mission on Coronavirus Disease 2019 (COVID-19), World Health Organization, 16-24 February 2020
- Chinese Center for Disease Control and Prevention. The Epidemiological Characteristics of an Outbreak of 2019 Novel Coronavirus Diseases (COVID-19), CCDC Weekly, 2(8):113-122, 2020.
- Wang C et al. A novel coronavirus outbreak of global health concern. Lancet, 395(10223): 470-473, 2020.
Global Allied Pharmaceuticals
1800, Pembrook Drive,
Orlando, FL 32810
United States of America.
Email: info@TakeChargeMedical.com
www.TakeChargeMedical.com

 Regulatory, Compliance, and
More.
Regulatory, Compliance, and
More.